About Allergy
Improving the knowledge about allergies and associated risks
Millions of people around the world suffer from allergies. In Europe, up to 25 percent of the population are affected by this condition. The numbers are rapidly increasing – in developed and in developing countries – with especially high incidence rates among children.
Although allergies can have a huge impact on a person’s quality of life, they are often perceived as a minor disorder. If treated at all, most of the patients receive only symptomatic treatment that is not targeting the underlying cause of the disease – the inadequately responding immune system.
At Allergopharma, we believe that allergies require an integrated health approach, involving early diagnosis and causal treatment of the condition. To achieve this, it is crucial to implement strategies to improve the knowledge about allergies in patients, physicians and healthcare providers and to raise awareness about the risks associated with the condition.
Most importantly, patients have to be aware that an allergy is a progressive disease: Allergy starts with the sensitization to one or more allergen molecules from an allergen source. The first allergic reaction occurs once the patient is re-exposed to these allergens. Over time, the allergic reaction can get stronger, patients are likely to get sensitized to additional allergens and may eventually develop an allergic asthma. Thus, allergies are associated with an increased risk for a life threatening disease. According to the World Health Organization (WHO), approximately 250,000 people die prematurely each year from asthma and almost all of these deaths are avoidable.
Presently, the only way to prevent a potential worsening and progression of the condition is an allergen immunotherapy (AIT). The systemic applications of allergens causing the allergic reaction have shown to de-sensibilize the immune system of a patient, so that he or she becomes more and more insensitive to these substances. For this, a patient receives increasing doses of an allergen over three years, resulting in a dramatic, long lasting drop of the symptoms or even a cure.
A holistic view on allergies
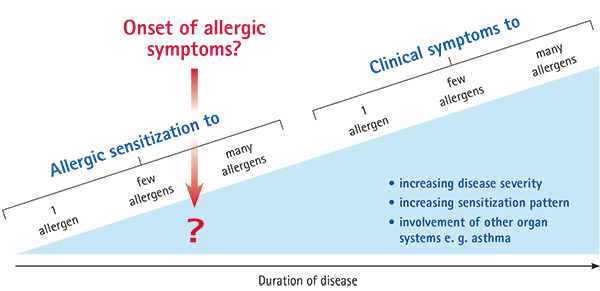
An allergy is typically described simplistic as a false reaction of the immune system to a substance that is normally harmless to the human body. At Allergophama we believe that allergies require a more holistic point of view: We define allergy as a systemic and progressive disorder with many different immunologic mechanisms involved.
Depending on genetic prepositions and environmental factors, these mechanisms can lead to initial sensitization to one or more allergen molecules, followed by further sensitizations to additional allergen molecules including different allergen sources. Exposure to these allergens causes an allergic reaction with local inflammation. Over time, the local allergen-driven inflammation can lead to chronic persistent inflammation and the manifestation of chronic asthma.
IgE-mediated allergies - type I allergic reactions
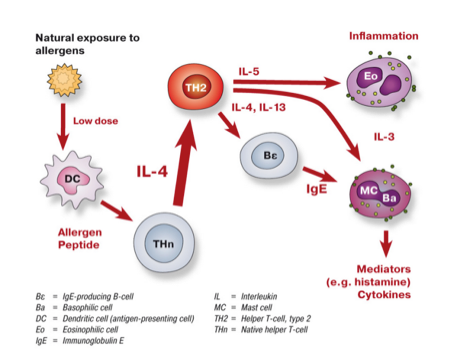
In IgE-mediated immediate reactions, there is an imbalance between the T-helper cell (TH) subpopulations of TH1 and TH2 cells. The two cell types release different cytokines that are important for the production of antibodies. In type I allergy patients there is an increased number of TH2 cells and a reduced TH1 reaction.
Following specific stimulation by an antigen or allergen, TH1 cells release cytokines (messenger substances) which cause B-cells to predominantly produce IgG antibodies. TH2 cells, however, cause an increased IgE synthesis, which is normally elicited by external parasites. In addition, allergy patients exhibit a relative deficiency of regulatory T cells (T-regs), which reduces the tolerance of the immune system to allergens.
After entering the human body, the allergen is taken up by an antigen-presenting cell, which breaks it down into smaller fragments, and presents some of these fragments to allergen-specific TH2 cells. Cytokines produced by the TH2 cells stimulate B cells to proliferate and differentiate into IgE-producing plasma cells. The secreted IgE binds to receptors on mast cells, with characteristic granulates containing histamine and other inflammatory mediators. The patient is now sensitized to the allergen.
Upon a following exposure, the allergen binds to the IgE antibodies on the mast cells. Within seconds, the mast cells release histamine and other mediators of the inflammatory response, triggering the allergic symptoms.